Transcatheter Aortic Valve Replacement (TAVR) is a procedure that remedies aortic stenosis to restore proper blood flow from the heart. Less commonly, TAVR can also be used to treat aortic regurgitation, a condition where the aortic valve does not close completely and causes blood to leak back into the left ventricle. Developed as an alternative to traditional open-heart surgical approaches, TAVR offers significant advantages, particularly for patients considered high-risk or unsuitable for conventional surgery due to various factors such as age or anatomical complexities. 40 to 45% of TAVR patients are discharged the same day as the procedure.
Figure A (Right)- A commonly used artificial heart valve.

What is Aortic Stenosis?
Aortic stenosis is a condition where the aortic valve does not fully open, restricting the flow of blood from the heart to the aorta and the rest of the body. The primary causes include age-related wear and tear, congenital defects, rheumatic fever, and past radiation therapy. Common symptoms include shortness of breath, chest pain, fatigue, and sometimes fainting, particularly during physical exertion. A heart murmur is often detectable via a stethoscope and serves as a key diagnostic indicator.
Calcium plays a pivotal role in the progression of aortic stenosis through a process known as calcification. Damage to the aortic valve leaflets—due to age, high blood pressure, or other factors—creates focal points for calcium deposits. Over time, these calcium phosphate crystals accumulate and harden the valve leaflets, causing them to become stiff and less flexible. This calcification narrows the valve and impairs its function, resulting in the heart needing to work harder to pump blood, which can lead to severe complications if left untreated.
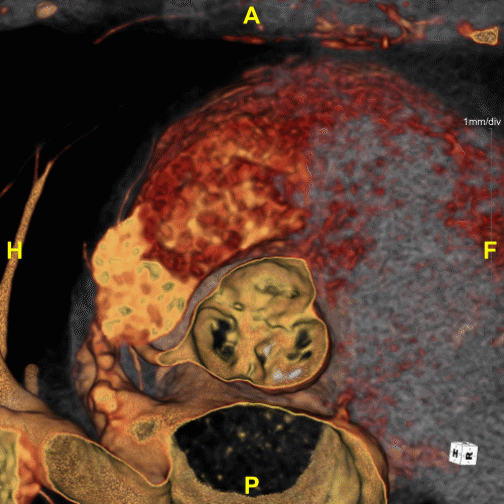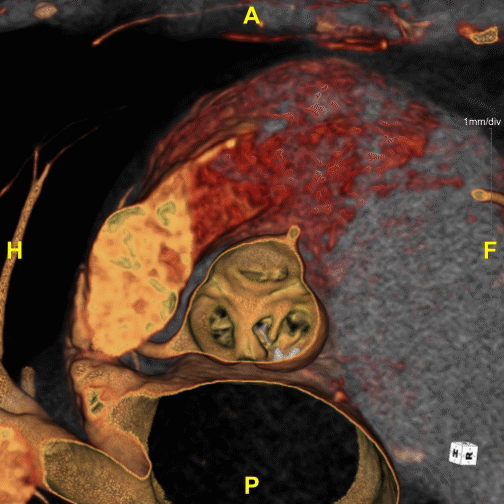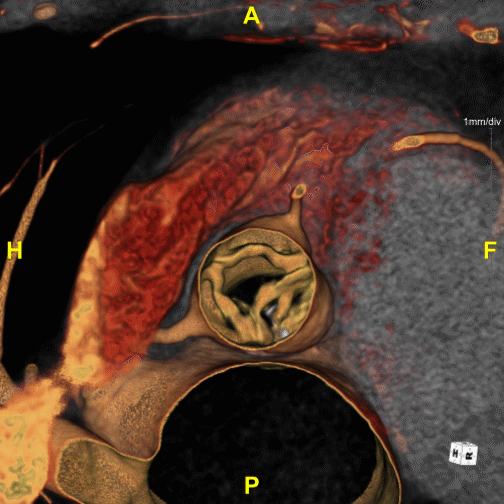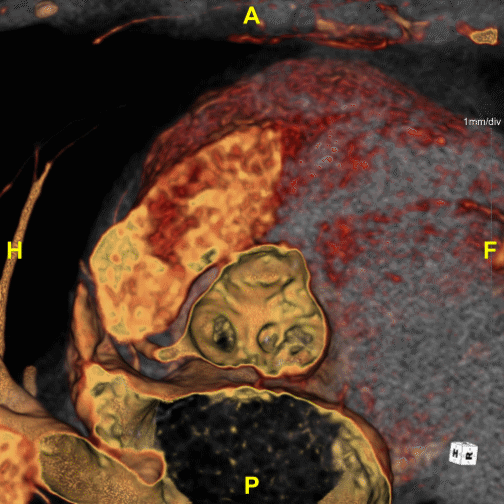
Figure B (Left) – Example of aortic stenosis: The lower right leaflet is demonstrating reduced movement.
How is TAVR performed?
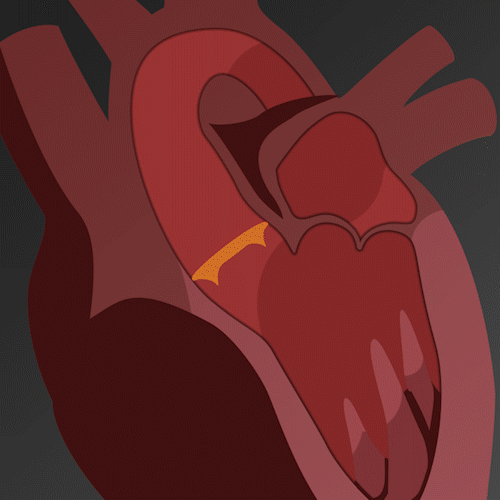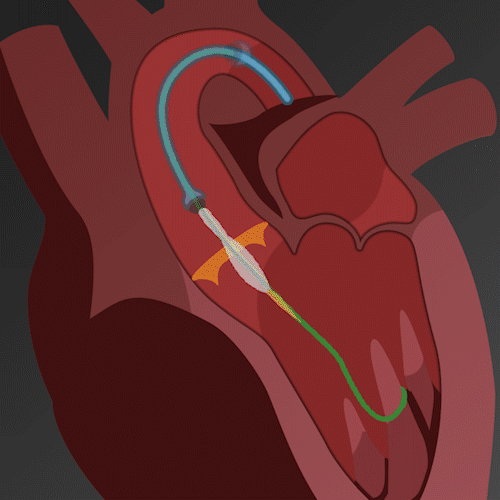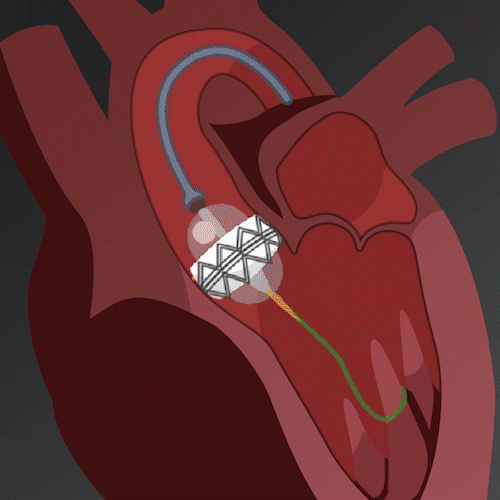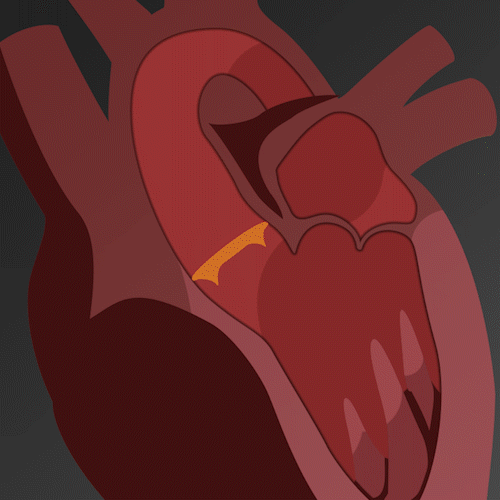
The TAVR procedure is performed by a specialized team of cardiology experts and cardiovascular surgeons. After administering local anesthesia and possibly sedation to the patient, a small incision is made, commonly in the groin area, to gain vascular access. A catheter equipped with a compressed artificial valve is then inserted through this incision and the accessed vessel. Utilizing real-time imaging for guidance, the team navigates the catheter through the vascular system until it reaches the defective aortic valve.
Once in the correct position, the artificial valve is expanded to replace the diseased valve, either by inflating a balloon or via a self-expanding mechanism. The valve starts functioning immediately, regulating the blood flow from the heart to the aorta. Finally, the catheter is withdrawn, and the incision is closed. Due to its minimally invasive nature, TAVR generally has a shorter recovery time compared to traditional open-heart surgery.
Figure C (Right) – Image series demonstrating the TAVR process.
Measurements
Before undergoing surgery, a gated computed tomography angiography (CTA) scan with a contrast agent is performed to visualize the heart’s blood flow. This data allows for the evaluation of Transcatheter Heart Valve (THV) dimensions and vessel access points, used to help determine the valve’s morphology, gauge the size and shape of the annulus—the base of the heart valve—and assess nearby coronary arteries and other cardiac structures. Iliac arteries are measured for TAVR access; if they are tortuous or narrow, the carotid or subclavian vessels are used instead. Ultimately, these measurements are used to select the most suitable prosthetic valve size, fine-tune the procedural plan, and minimize associated risks and complications. Below are measurements commonly provided by the 3DQ Lab for TAVR patients:
Figure D (Right) – Possible locations used for TAVR access: Iliacs, Carotid, and Subclavian.

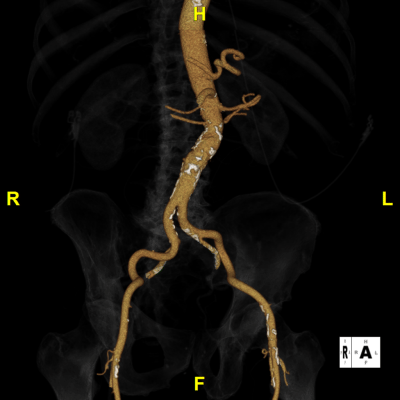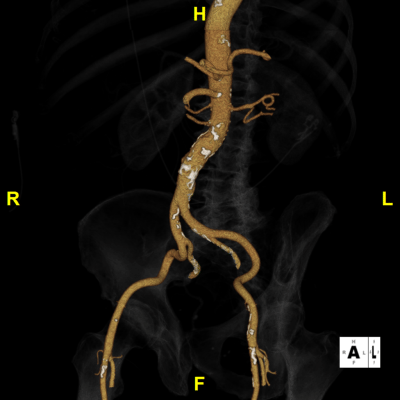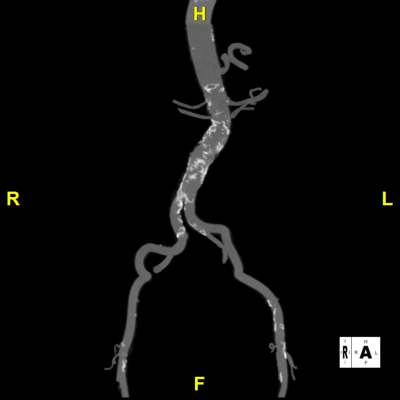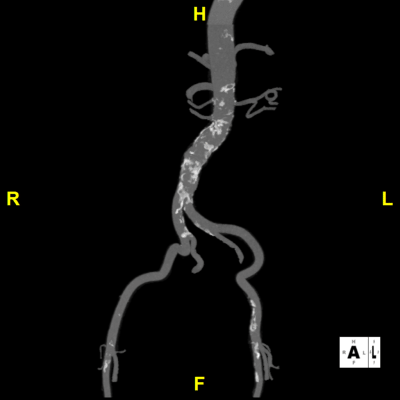
Figure E: Rotational Iliac – Used for determining suitable catheter access points and identifying potential vascular complications.

Figure F: Iliac Measurements – Artery diameter and length are important when selecting the appropriate catheter and delivery system.

Figure G: THV Curved Planar Reconstructions (CPRs) – Provide entire length views of the access vessels, indicating areas of tortuous or calcified structures.
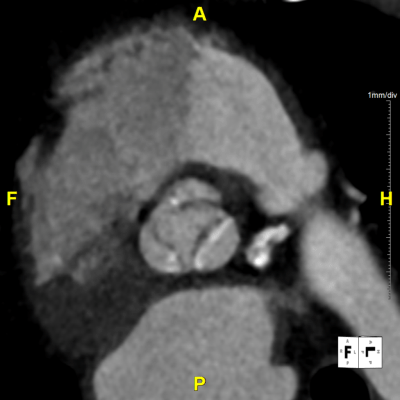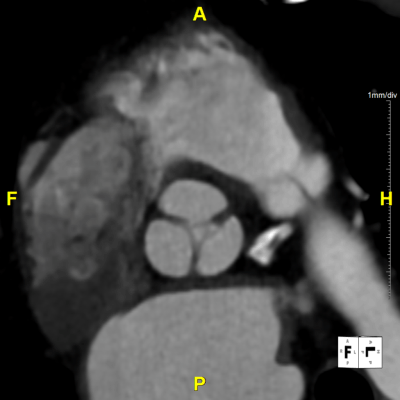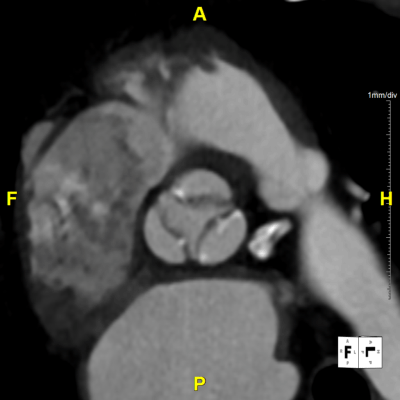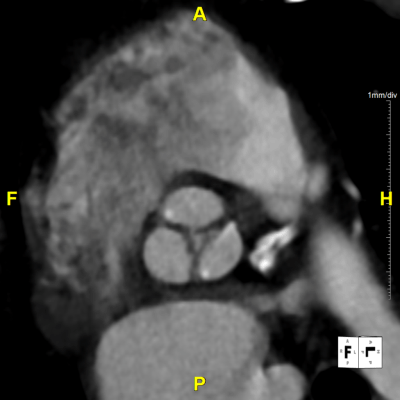
Figure H: En Face Video – Provides a “birds-eye-view” directly at the plane of the aortic valve, demonstrates the valve and nearby structures in motion.
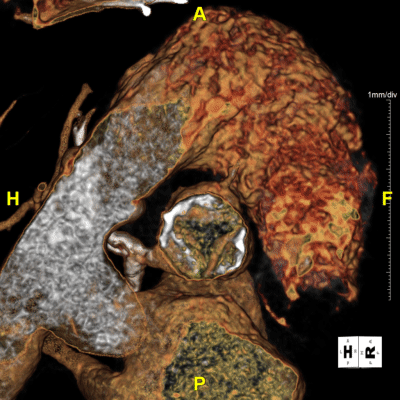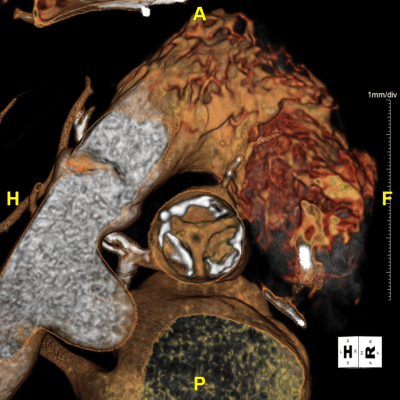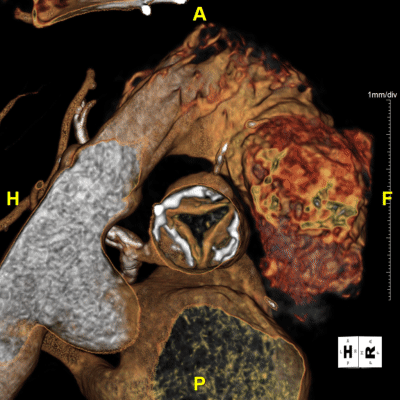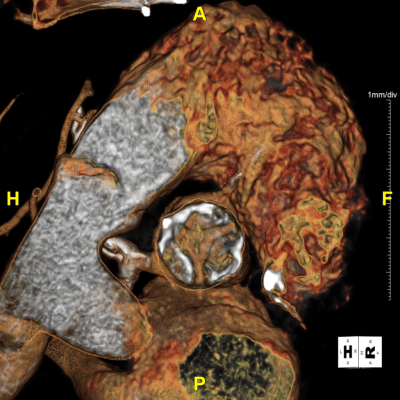
Figure I: 4D-Valve Movie – Useful for understanding the valve’s functional behavior, such as leaflet motion and blood-flow patterns that static images can’t capture.

Figure J: Coronary Curved Planar Reconstructions (CPRs) – Provide a detailed 2D review of the 3D structure of the coronary arteries, ensuring complications like coronary artery obstruction are not missed.
Benefits of TAVR
• Reduced Surgical Impact: TAVR is minimally invasive, requiring only a small incision. This leads to shorter hospital stays and quicker recovery periods compared to traditional surgery.
• Expanded Patient Access: The procedure offers a lifesaving option for those deemed unsuitable for standard surgical approaches due to age or pre-existing health conditions.
• Improved Quality of Life: Post-procedure, patients often experience significant improvements in symptoms and physical capabilities, enhancing their overall quality of life.
Risks and Considerations
• Longevity Concerns: Questions about the long-term durability of transcatheter valves as opposed to surgical valves still exist, although ongoing research aims to address this.
• Procedure-related Complications: Like any surgical procedure, TAVR has associated risks including bleeding, vascular issues, and the possibility of stroke. However, technological advancements are mitigating these risks.
• Financial Constraints: TAVR can be costly, and insurance coverage may vary, potentially limiting accessibility for some individuals.
3DQ Lab – Grant Building
3DQ Lab – Clark Building
Learn More About the Lab
Copyright © Stanford University